Impact of the COVID-19 Pandemic on Obesity in Children and Adolescents
ABSTRACT
The outbreak of the COVID-19 pandemic has necessitated a number of restrictions, including movement limitations and the closure of educational establishments. The shift to remote learning and staying at home during the hard times of the pandemic contributed to adverse consequences for children and adolescents. It is reported that during the pandemic there was a significant increase in eating disorders and the problem of overweight and obesity. This has been shown to be related to poor mental health, but also boredom and sedentary lifestyles. The restrictions implemented during the COVID-19 pandemic reduced the transmission of coronavirus. Nevertheless, according to the study, these restrictions exacerbated risk factors for the development of another epidemic - the obesity epidemic. As a result, we are likely to experience an increase in the number of people with obesity-related diseases in the future. However, it is important to remember that overweight and obesity can be combated, but this is more difficult to achieve in adulthood. An attempt should therefore be made to make society aware of the consequences of obesity and overweight. Furthermore, a physically and mentally healthy lifestyle should be promoted among children and adolescents.
KEYWORDS
Children; Adolescents; Obesity; Covid-19; Pandemic
INTRODUCTION
Coronavirus Pandemic Disease 2019 (COVID-19) has caused fundamental changes in many areas of life [1,2]. The rapid increase in the number of infections, the lack of effective drugs, the oftensevere course of the disease and the high mortality rate have led to an overburdened health sector. In order to stop the rapid spread of the disease, restrictions were inevitable. These consisted of restricting the operation of many sectors of the economy and closing educational establishments [2-4]. Pandemic COVID-19 has been proven to have a significant impact on the emotional and social development of children and adolescents [4]. Restrictions may have increased rates of childhood obesity [5,6]. For the young population, isolation became a cause of anxiety and fear for the health of themselves and family members. It was also associated with difficulty in making social contacts [7,8]. Sudden isolation from peers, friends and grandparents, as well as the experience of the death of a relative had an impact on emotional disruption and loneliness [4]. Anxiety, irritability, stress, feelings of boredom and the necessity to stay at home for long periods of time may have contributed to the severity of eating disorders in children and adolescents [5,9]. Compensating for negative emotions, many children have started to consume tasty, highly processed and caloric foods, thus abandoning a properly balanced diet [5,10-12]. The remote learning should also be taken into account, as well as a lack of exercise in leisure time. More time spent in front of the computer/television has also encouraged snacking. The addictive aspects of salty and sweet snacks have been reported by many sources [11,13]. The addiction itself has implications for long-term change in eating habits. Furthermore, overweight and obesity are predicted to worsen in patients diagnosed before the pandemic [14-16]. Difficult access to medical personnel during the COVID-19 pandemic may have delayed the diagnosis and implementation of treatment for patients with eating disorders and obesity. Isolation was also associated with a reduction in the number of followup visits, while the number of visits is associated with greater treatment efficacy [14,16,17].
According to the WHO (World Health Organization), overweight and obesity is, “abnormal or excessive fat accumulation that can harm health” [18]. Childhood obesity is one of the most serious health problems of the 21st century [19]. Even moderate overweight in childhood significantly increases the risk of developing type 2 diabetes and cardiovascular disease in middle age [20]. In obese children, the development of these diseases is even more common and the risk of premature death and disability in adulthood is increased [19,21]. The purpose of this article is to highlight and briefly discuss the growing problem of overweight and obesity in the child and adolescent age group during the COVID-19 pandemic.
MAIN TEXT
Jenssen et al. [6] conducted a large study involving patients aged 2 to 7 years. It included urban, semi-urban and semi-rural centers in the Philadelphia region (PA, USA). The study aimed to compare childhood obesity in the pre-pandemic period and during the COVID-19 pandemic. For this purpose, the period from June to December 2019 (pre-pandemic period) and the period from June to December 2020 (pandemic) were considered as representative months. An increase in the average prevalence of obesity was observed in every age group already at the beginning of the pandemic. On average, the overall prevalence of obesity among the children surveyed increased from 13.7% to 15.4%. The greatest increase occurred in the population of children aged 5 to 9 years - an increase of 2.6% [6].
A study by Yang et al. [22] assessed the change in obesity and overweight rates among Chinese high school students by comparing data from one month before the pandemic (December 2019) with data collected one month after the introduction of lockdown (February 2020). For two months, the percentage of obese people among the study population increased by 2.8%, while the percentage of overweight people increased by 3.7%.
The results of the above studies seem to be in agreement with the hypothesis that the risk of childhood obesity is increased in the outof- school months [3,15,23,24]. This trend is favored by factors such as reduced physical activity, prolonged sedentary time, increased time spent in front of screens (TV, computer, smartphones etc.), irregular circadian rhythm, poor quality of sleep, snacking (often on sugary or high-fat products), skipping breakfast [3,6,10,15,20]. Children and adolescents appear to be even more vulnerable to the above factors during the COVID-19 pandemic than during the holiday season.
In France, after the introduction of lockdown, a study was conducted which showed that 26.2% of respondents claimed to have lost control over their daily eating habits [5]. This correlated significantly with food consumption to alleviate feelings of emptiness, stress and boredom [5]. The frequent association of eating disorders with mental disorders therefore appears to have been of greater concern during the pandemic, as there was an increase in the number of people reporting mental health problems [5,9,25].
In China, the percentage of adolescents reporting depressive symptoms increased by 22.6% [25]. Such a fact is all the more important given the frequent coexistence of obesity and depression [26]. Taking into account this interdependence of these two diseases, Mediouni et al. [26] proposed the new term “depreobesity”. Thus, the negative effects of restrictions on gathering and movement, as well as the shift to distance learning in terms of depressogenic and overweight-promoting effects, may be mutually exacerbating.
The COVID-19 pandemic placed an immediate strain on the health care system. As a result, many mental health and obesity/ overweight treatment centers were converted to care for COVID-19 patients. In addition, consultations were restricted to urgent cases [14,25]. Thus, poor access to treatment during the pandemic made diagnosis difficult and probably exacerbated the health problem of children and adolescents with eating disorders and/or obesity diagnosed before the pandemic [14,15].
In their study, Pietrobelli et al. [15] attempted to determine whether factors contributing to weight gain were exacerbated during lockdown. The study included 41 individuals aged between 6 and 18 years. Juxtaposing the 2019 data with data collected after 3 weeks of isolation showed that negative health habits were significantly escalated during the pandemic. Among the food aspects, there was a 27.58% increase in the number of meals consumed per day, a 92.22% increase in the consumption of red meat, a 771.43% increase in the consumption of crisps and a 125% increase in the consumption of sugary drinks [15]. In terms of physical activity, there was a significant increase in time spent in front of a screen and a decrease in time spent exercising [15].
Similarly, Ruiz-Roso et al. [27] in their study demonstrated that during COVID-19 physical activity levels decreased and consumption of ultra-processed foods increased among adolescents. It has been speculated that decreased physical activity may exacerbate depressive symptoms in children [25]. The fact that poor mental health may contribute to the development of overweight and obesity has already been mentioned. Thus, it seems reasonable to view these phenomena as a self-perpetuating vicious circle.
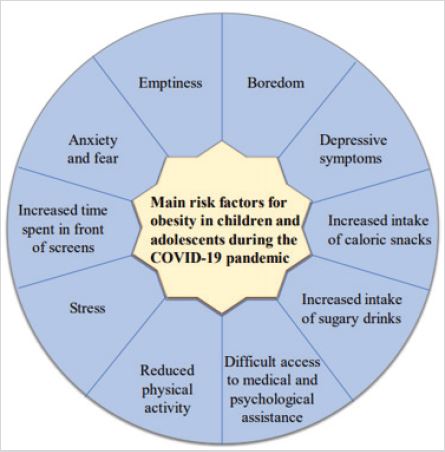
WHO data from before the COVID-19 pandemic indicated a worrying state of overweight and childhood obesity rates [18]. During the pandemic, when the effects contributing to overweight were exacerbated, obesity rates in children and adolescents appear to have worsened even further [28]. The health consequences of childhood obesity span multiple systems [29,30]. An elevated BMI (body mass index) is recognized by WHO as a major risk factor for non-communicable diseases such as cardiovascular disease, musculoskeletal disease, diabetes or malignancy [18,20]. Usually, cardiovascular complications of obesity occur in later life. However, pathological changes in the form of atherosclerosis, left ventricular hypertrophy or hypertension can already be observed in childhood [30-32]. Furthermore, obesity causes harmful consequences including pulmonological, orthopedic, endocrinological, immunological and gastroenterological, as well as psychological effects [18,20,29]. Figure 1 shows the main factors associated with the COVID-19 pandemic that contribute to the increased problem of overweight and obesity in children and adolescents.
CONCLUSION
Available research shows that the COVID-19 pandemic increased risk factors for childhood overweight and obesity. Children and adolescents forced to stay at home consumed more highly processed foods and more sweetened drinks. This, combined with reduced physical activity, was associated with weight gain. Psychological aspects such as feelings of emptiness, anxiety, fear, loneliness and boredom, which were often compensated by eating, may have an indirect effect on the increased rates of overweight and obesity in this population. Particular attention should be paid to the fact that health habits acquired in childhood, including nutritional and physical activity habits, may be maintained in later life. As a result, unfavorable habits can exacerbate the development of serious diseases affecting, among others, the cardiovascular and respiratory systems. They may also be associated with an increased risk of cancer and diabetes. Often, obese children become obese adults, and as is generally known, obesity is more difficult to treat in adulthood.
Before the COVID-19 pandemic, obesity and overweight among children and adolescents was a global problem. The problem began to grow more rapidly during the pandemic. It is therefore necessary to take decisive steps to raise public awareness of the scale of the problem of overweight and obesity. It is difficult to require parents to have constant control over their children’s meals. Nevertheless, they should consciously buy products and limit highly processed snacks, sweetened drinks and other high-calorie foods. It is important that people struggling with eating disorders, overweight, obesity and mental health problems have continued access to treatment, such as through telemedicine. Online discussions with school psychologists can also be helpful and should be easily accessible. In addition, children and young people should be encouraged to be more physically active. During a pandemic, exercise can be done at home, for example, in the form of play.
REFERENCES
- Wadolowska L, Drywien M, Hamulka J, Socha P, Borawska M, et al. (2021) Zalecenia zywieniowe podczas pandemii COVID-19. Stanowisko komitetu nauki o zywieniu czlowieka polskiej akademii nauk. Standardy Medyczne 18: 289-298.
- Ammar A, Brach M, Trabelsi K, Chtourou H, Boukhris O, et al. (2020) Effects of COVID-19 home confinement on eating behaviour and physical activity: Results of the ECLB-COVID19 International Online Survey. Nutrients 12(6): 1583.
- Rundle AG, Park Y, Herbstman JB, Kinsey EW, Wang YC (2020) COVID-19 related school closings and risk of weight gain among children. Obesity (Silver Spring) 28(6): 1008-1009.
- Singh S, Roy D, Sinha K, Parveen S, Sharma G, et al. (2020) Impact of COVID-19 and lockdown on mental health of children and adolescents: A narrative review with recommendations. Psychiatry Res 293: 113429.
- Cherikh F, Frey S, Bel C, Attanasi G, Alifano M, et al. (2020) Behavioral food addiction during lockdown: Time for awareness, time to prepare the aftermath. Obes Surg 30(9): 3585-3587.
- Jenssen BP, Kelly MK, Powell M, Bouchelle Z, Mayne SL, et al. (2021) COVID-19 and changes in child obesity. Pediatrics 147(5): e2021050123.
- Sidor A, Rzymski P (2020) Dietary choices and habits during COVID-19 lockdown: Experience from Poland. Nutrients 12(6): 1657.
- Loades ME, Chatburn E, Higson SN, Reynolds S, Shafran R, et al. (2020) Rapid systematic review: The impact of social isolation and loneliness on the mental health of children and adolescents in the context of COVID-19. J Am Acad Child Adolesc Psychiatry 59(11): 1218-1239.
- Puzio A, Biskupek WA, Wanot B (2020) Eating disorders. In: Diet and health and age. Scientific Publishers of the University of Humanities and Life Sciences, Jan Długosz in Częstochowa, pp. 144-154.
- Nicodemo M, Spreghini MR, Manco M, Wietrzykowska SR, Morino G (2021) Childhood obesity and COVID-19 lockdown: Remarks on eating habits of patients enrolled in a food-education program. Nutrients 13(2): 383.
- Yau YHC, Potenza MN (2013) Stress and eating behaviors. Minerva Endocrinol 38(3): 255-267.
- Coulthard H, Sharps M, Cunliffe L, van den Tol A (2021) Eating in the lockdown during the Covid 19 pandemic; self-reported changes in eating behaviour and associations with BMI, eating style, coping and health anxiety. Appetite. 161: 105082.
- Cummings JR, Joyner MA, Gearhardt AN (2020) Development and preliminary validation of the anticipated effects of food scale. Psychol Addict Behav 34(2): 403-413.
- Todisco P, Donini LM (2021) Eating disorders and obesity (ED & amp; O) in the COVID-19 storm. Eat Weight Disord - Stud Anorexia, Bulim Obes 26(3): 747-750.
- Pietrobelli A, Pecoraro L, Ferruzzi A, Heo M, Faith M, et al. (2020) Effects of COVID‐19 lockdown on lifestyle behaviors in children with obesity living in Verona, Italy: A longitudinal study. Obesity 28(8): 1382-1385.
- Touyz S, Lacey H, Hay P (2020) Eating disorders in the time of COVID-19. J Eat Disord 8(1):19.
- Smith JD, Fu E, Kobayashi MA (2020) Prevention and management of childhood obesity and its psychological and health comorbidities. Annu Rev Clin Psychol 16: 351-378.
- WHO (2021) Obesity and overweight.
- WHO (2021) Obesity.
- Weihrauch BS, Wiegand S (2018) Risk factors and implications of childhood obesity. Curr Obes Rep 7(4): 254-259.
- The WHO European childhood obesity surveillance initiative (2018) Factsheet: Childhood obesity Surveillance initiative, Highlights 2015-17.
- Yang S, Guo B, Ao L, Yang C, Zhang L, et al. (2020) Obesity and activity patterns before and during COVID‐19 lockdown among youths in China. Clin Obes 10(6).
- von Hippel PT, Workman J (2016) From kindergarten through second grade, U.S Children’s obesity prevalence grows only during summer vacations. Obesity 24(11): 2296-2300.
- Franckle R, Adler R, Davison K (2014) Accelerated weight gain among children during summer versus school year and related racial/ethnic disparities: A systematic review. Prev Chronic Dis 11: 130355.
- Nicolini H (2020) Depresión y ansiedad en los tiempos de la pandemia de COVID-19. Cir Cir 88(5): 542-547.
- Mediouni M, Kaczor UKE, Madiouni R (2020) Future epidemic: Depreobesity. Obes Med 100240.
- Ruíz RMB, de Carvalho Padilha P, Matilla-Escalante DC, Brun P, Ulloa N, et al. (2020) Changes of physical activity and ultra-processed food consumption in adolescents from different countries during Covid-19 pandemic: An observational study. Nutrients 12(8): 2289.
- Clemmensen C, Petersen MB, Sørensen TIA (2020) Will the COVID-19 pandemic worsen the obesity epidemic? Nat Rev Endocrinol 16(9): 469- 470.
- Jolanta N, Zbigniew B (2019) Epidemia otyłości dzieci w 2. dekadzie XXI w. w Polsce i w Europie. Aspekt medyczny i aspekt ekonomiczny problematu. 47(1).
- Nogueira-de-Almeida CA, Del Ciampo LA, Ferraz IS, Del Ciampo IRL, Contini AA, et al. (2020) COVID-19 and obesity in childhood and adolescence: a clinical review. J Pediatr (Rio J) 96(5): 546-558.
- Berenson GS (2012) Health consequences of obesity. Pediatr Blood Cancer 58(1): 117-121.
- Artur M, Ewelina R, Katarzyna M, Maria R, Damian M (2008) Prevalence of overweight and obesity in preschool children from Rzeszow region. Endocrinology, Obesity and Metabolic Disorders 4(4): 159-162.
Article Type
Review Article
Publication history
Received date: September 03, 2021
Published date: September 22, 2021
Address for correspondence
Hubert Mado, Department of Histology and Cell Pathology in Zabrze, Medical University of Silesia in Katowice, Poland
Copyright
©2021 Open Access Journal of Biomedical Science, All rights reserved. No part of this content may be reproduced or transmitted in any form or by any means as per the standard guidelines of fair use. Open Access Journal of Biomedical Science is licensed under a Creative Commons Attribution 4.0 International License
How to cite this article
Kisielewska W, Mado H. Impact of the COVID-19 Pandemic on Obesity in Children and Adolescents. 2021- 3(5) OAJBS.ID.000321.